
Understanding Type 2 Diabetes — What It Is, Why It Matters, and How to Take Control
Type 2 diabetes is one of the fastest-growing health conditions in the UK — a chronic but manageable illness that affects how your body regulates sugar (glucose) in the bloodstream.
Although millions live with it every day, its causes, management and impact are still misunderstood.
In this post, we’ll explore the facts, lifestyle solutions, and empowering steps you can take to live well.
What Is Type 2 Diabetes?
Type 2 diabetes occurs when your body becomes resistant to insulin — the hormone made by the pancreas that helps turn glucose from food into energy.
Over time, the pancreas can’t produce enough insulin to overcome that resistance, allowing sugar to build up in the blood.
This long-term rise in blood sugar can damage blood vessels, organs and nerves, leading to serious health problems if not managed correctly.
In the UK, around 4.3 million people are living with diabetes, of which about 90% have Type 2 (Source: Diabetes UK, 2026).
The number continues to rise, driven by changing lifestyles, ageing populations, and increased awareness and testing.
Who Is Affected?
Anyone can develop Type 2 diabetes, but several risk factors make some people more vulnerable:
- Age: It’s more common after 40, but younger cases are increasing.
- Family history: If a close relative has it, your risk rises.
- Ethnicity: South Asian, Black African and Caribbean communities face a higher risk.
- Body weight: Carrying excess weight, especially around the waist, is one of the strongest predictors.
- Inactive lifestyle: Sedentary habits reduce insulin sensitivity.
- Diet: Frequent consumption of high-sugar, processed and high-fat foods contributes heavily.
There’s no single blueprint.
Many people have a combination of genetic predisposition and environmental factors that interact over time.
For example, someone with a family history who gains weight in midlife can tip into diabetic territory after years of quiet change.
Why It Matters

Untreated or poorly managed Type 2 diabetes can have broad consequences. Persistently high blood sugar damages the circulatory system, increasing the risk of:
- Heart disease and stroke
- Vision problems (diabetic retinopathy)
- Nerve damage (neuropathy)
- Kidney disease
- Slow-healing wounds and infections
Beyond these medical risks, the condition also affects daily life, from energy levels and sleep patterns to emotional well-being.
Managing diabetes effectively can prevent or delay these effects and allow a full, active lifestyle.
Where It Begins — Early Signs and Diagnosis
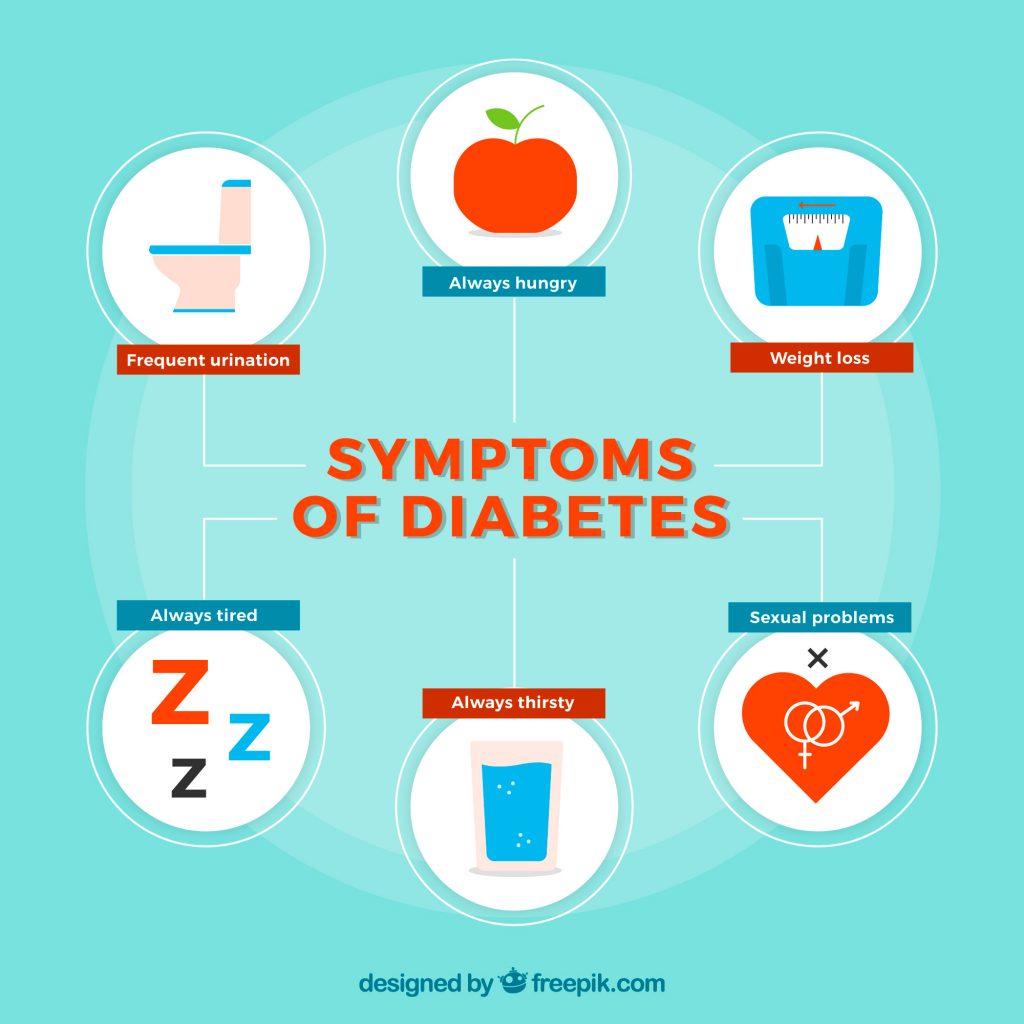
Early signs can be subtle, but catching them matters.
Common symptoms include:
- Increased thirst and frequent urination
- Fatigue
- Unexplained weight loss
- Blurred vision
- Slow-healing cuts or infections
- Tingling hands or feet
If these sound familiar, a simple blood test through your GP or local NHS screening can confirm your glucose and HbA1c levels (your average blood sugar over three months).
Diagnosis usually involves one or more of these tests and may lead to regular monitoring with a diabetes care team.
When It Develops — The Timeline of the Condition
Type 2 diabetes doesn’t appear overnight.
It’s often the result of years of insulin resistance quietly increasing — a stage known as prediabetes.
At this point, blood sugar levels are higher than normal but not yet high enough for diagnosis.
This progression can sometimes be reversed through lifestyle changes, particularly diet adjustments and increased physical activity.
Catching diabetes early, or even before it starts, can make a world of difference.
How to Manage and Improve Type 2 Diabetes
The good news is that Type 2 diabetes can be manageable and sometimes even reversible through consistent lifestyle decisions and medical support.
The NHS emphasises six core pillars of management:
1. Balanced Diet
Focus on low-glycaemic foods that release sugar slowly.
Emphasise:
- Whole grains, legumes and vegetables
- Lean proteins such as fish, chicken, tofu
- Healthy fats (olive oil, nuts, seeds)
- Limiting sugary drinks and refined carbs
A Mediterranean-style eating pattern is often recommended, rich in fibre and healthy fats.
2. Physical Activity
Regular movement enhances insulin sensitivity.
Even modest activity helps:
- Aim for 150 minutes per week of moderate exercise (walking, swimming, cycling).
- Strength training twice weekly supports muscle glucose use.
- Short, frequent walks after meals stabilise blood sugar peaks.
3. Weight Management
Even losing 5–10% of body weight can considerably improve blood sugar control.
The NHS provides structured programmes and local group sessions designed to aid long-term success.
4. Medication
Sometimes lifestyle changes aren’t enough initially.
Common prescriptions include:
- Metformin: improves insulin sensitivity and reduces liver glucose output.
- GLP-1 receptor agonists: support insulin production and satiety.
- Insulin: only required when other measures fail to maintain balance.
A healthcare team tailors the regimen depending on your response and lab results.
5. Regular Monitoring
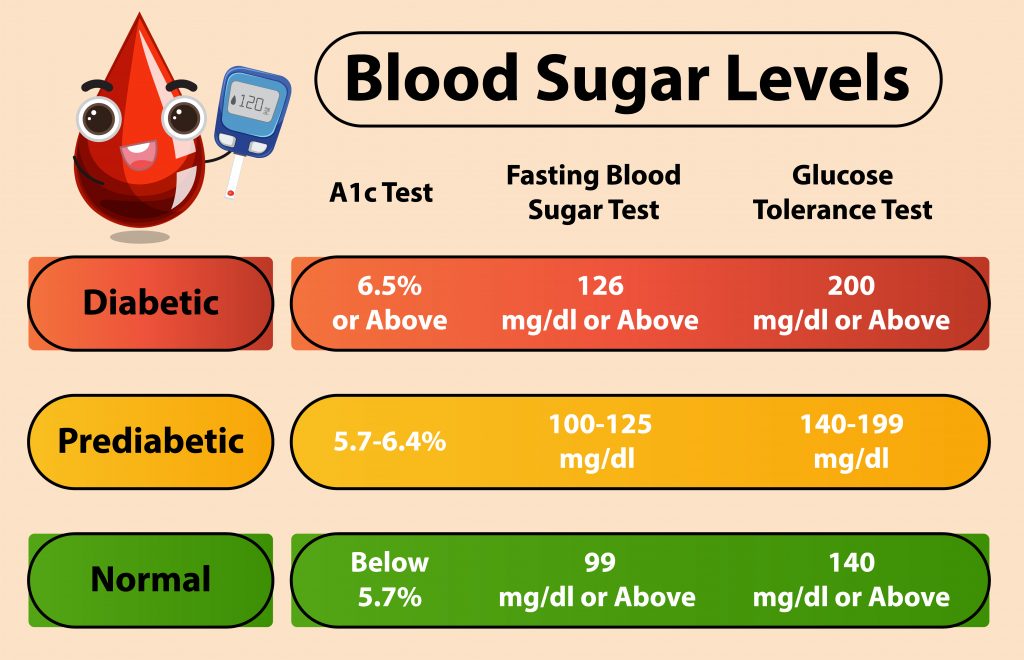
Check your HbA1c levels at least twice yearly, monitor blood pressure and cholesterol, and keep an eye on feet, eyes and kidneys.
The NHS offer free blood glucose meters to patients so that they can monitor their glucose levels. There is no need to purchase a meter, as manufacturers provide them free of charge to GP surgeries and clinics for distribution to patients.
Prevention is always better than damage repair.
6. Mental Health Care
Living with diabetes can be emotionally challenging. Stress, anxiety and depression can adversely affect blood sugar. Mindfulness, support groups and psychological therapy can help keep both mood and metabolism in good shape.
Lifestyle Example — Making It Real
Imagine John, a 45-year-old office worker from Leeds who used to enjoy late-night takeaways and rarely exercised.
After a diagnosis, he joined an NHS Diabetes Prevention Programme and began walking 30 minutes daily, swapped crisps for mixed nuts, and learned portion control.
Within nine months, he lost 12kg and his blood sugar dropped to prediabetic range — no medication required.
It’s not a miracle; it’s steady, evidence-based change applied consistently.
Living Well — The Ongoing Journey
Managing Type 2 diabetes isn’t about perfection; it’s about patterns.
Most people experience ups and downs, but long-term commitment to balanced choices pays off hugely.
The combination of self-management and NHS support services means there’s no need to face it alone.
If you’re looking for UK-based resources, here are some useful links:
- Diabetes UK — extensive guidance and local support groups.
- NHS Diabetes Services — detailed care pathways and prevention programmes.
- Low Carb Program — a digital app endorsed by NHS innovation partners.
Key Takeaways
Type 2 diabetes is not a punishment or a failure – it’s a signal.
It asks for a renewed relationship with your body, your habits, and your food.
With knowledge, structure and the right support, living well with diabetes is absolutely achievable. It starts with awareness, moves through daily action, and continues with lifelong empowerment.
